Gut Health and Immune System A Powerful Connection
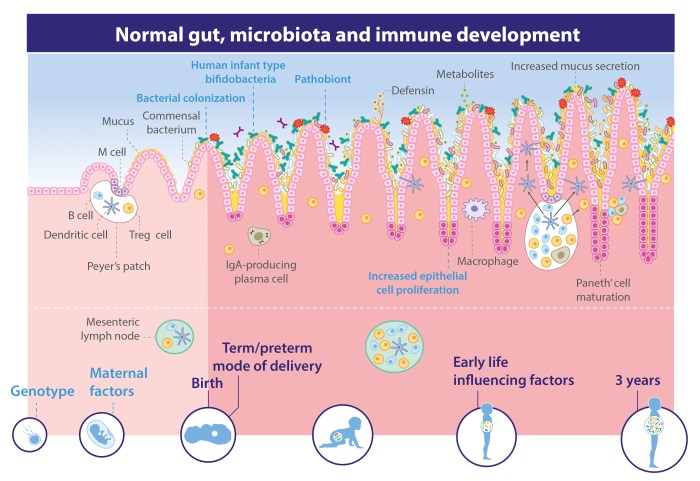
Gut health and immune system function are intricately linked. The trillions of microorganisms residing in our gut, collectively known as the gut microbiome, play a crucial role in shaping our immune responses. This complex interplay, a dynamic conversation between the gut and the immune system, profoundly impacts our overall health and susceptibility to disease. Understanding this connection is key to optimizing both gut health and immune function.
This exploration delves into the bidirectional communication between the gut microbiome and the immune system, examining how diet, lifestyle, and targeted interventions can influence this critical relationship. We’ll explore the impact of various dietary patterns, the benefits of specific foods and supplements, and the importance of lifestyle factors in fostering a healthy gut and a robust immune system. Ultimately, the goal is to empower you with knowledge and actionable strategies to enhance your well-being through a holistic approach to gut health.
The Gut-Immune System Connection
The gut and the immune system are intimately linked, engaging in a constant, dynamic crosstalk that profoundly impacts overall health. This bidirectional communication pathway involves a complex interplay between the gut microbiome – the trillions of bacteria, fungi, viruses, and other microorganisms residing in our digestive tract – and the components of our immune system. A healthy gut microbiome is crucial for the proper functioning of the immune system, while immune responses, in turn, shape the composition and activity of the gut microbiota.
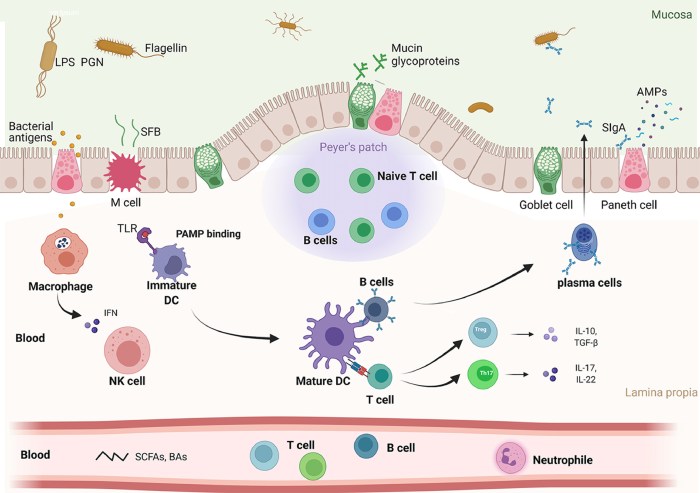
The gut microbiome influences immune responses through several mechanisms. The microbiota directly interacts with immune cells residing in the gut lining, such as macrophages and dendritic cells. These cells sample the microbial environment, and based on the signals they receive, they either promote tolerance to harmless bacteria or trigger immune responses against pathogens. Additionally, the gut microbiota produces a vast array of metabolites, such as short-chain fatty acids (SCFAs) like butyrate, propionate, and acetate.
These metabolites can modulate immune cell activity, influencing both innate and adaptive immune responses. For instance, SCFAs can promote the production of regulatory T cells (Tregs), which suppress excessive inflammation and maintain immune homeostasis. Conversely, dysregulation of these interactions can lead to detrimental consequences.
Mechanisms of Gut Microbiota Influence on Immune Responses
The gut microbiota influences immune responses through a variety of intricate mechanisms. These include direct interaction with immune cells, production of metabolites that modulate immune cell function, and indirect effects on the integrity of the gut barrier. The composition of the gut microbiota dictates the types and levels of these interactions, influencing the overall immune response. For example, a diverse and balanced microbiome tends to promote a balanced immune response, whereas an imbalanced microbiome (dysbiosis) can lead to chronic inflammation and immune dysfunction.
Specific bacterial species can produce molecules that either stimulate or suppress immune responses, highlighting the nuanced role of the microbiota in shaping immunity.
Examples of Gut Dysbiosis Contributing to Immune Dysfunction
Gut dysbiosis, an imbalance in the gut microbiota composition, is increasingly recognized as a contributing factor to various immune-related disorders. For example, reduced microbial diversity has been associated with inflammatory bowel disease (IBD), where an overactive immune response targets the gut lining. Similarly, alterations in the gut microbiota have been linked to autoimmune diseases like type 1 diabetes and rheumatoid arthritis.
In these conditions, an aberrant immune response directed against the body’s own tissues is thought to be partly driven by changes in the gut microbial community. Furthermore, dysbiosis has been implicated in the development of allergies and asthma, suggesting a broader impact on immune regulation. The disruption of the delicate balance between commensal bacteria and the immune system can result in various immune dysfunctions, emphasizing the importance of maintaining a healthy gut microbiome.
Comparison of Immune Responses in Healthy vs. Unhealthy Gut Microbiomes
| Characteristic | Healthy Gut Microbiome | Unhealthy Gut Microbiome (Dysbiosis) | Clinical Implications |
|---|---|---|---|
| Microbial Diversity | High; diverse range of bacterial species | Low; reduced diversity, potential dominance of harmful species | Increased risk of infections and immune disorders |
| Gut Barrier Integrity | Intact; effective barrier against pathogens | Compromised; increased permeability (“leaky gut”) | Chronic inflammation, autoimmune diseases |
| Immune Response | Balanced; appropriate responses to pathogens, tolerance to commensals | Dysregulated; chronic inflammation, exaggerated or suppressed responses | Inflammatory bowel disease, allergies, autoimmune diseases |
| Short-Chain Fatty Acid (SCFA) Production | High levels of SCFAs (butyrate, propionate, acetate) | Reduced SCFA production | Increased inflammation, impaired immune regulation |
Impact of Diet on Gut Health and Immunity
The intricate relationship between our diet and both gut health and immune function is undeniable. The food we consume directly influences the composition and activity of our gut microbiota – the trillions of bacteria, fungi, and other microorganisms residing in our digestive tract. This microbial ecosystem plays a crucial role in various bodily functions, including nutrient absorption, immune system development, and protection against pathogens.
A diet rich in specific nutrients can foster a thriving gut microbiome, bolstering our immune defenses, while an imbalanced diet can negatively impact gut health and increase susceptibility to illness.
The Role of Prebiotics and Probiotics in Supporting Gut Health and Immune Function
Prebiotics and probiotics are often discussed together, yet they have distinct roles in supporting gut health. Prebiotics are non-digestible food ingredients that act as “food” for beneficial bacteria in the gut, promoting their growth and activity. Examples include inulin, found in many fruits and vegetables, and resistant starch, present in foods like bananas and potatoes. Probiotics, on the other hand, are live microorganisms, typically bacteria or yeasts, that, when consumed in adequate amounts, confer a health benefit.
Common probiotic strains include
- Lactobacillus* and
- Bifidobacterium*, often found in yogurt, kefir, and fermented foods. Both prebiotics and probiotics contribute to a balanced gut microbiome, enhancing its ability to support immune function by strengthening the gut barrier, modulating immune cell activity, and preventing the growth of harmful bacteria. A diet incorporating both prebiotics and probiotics is crucial for maintaining optimal gut health and a robust immune system.
Dietary Patterns and Their Effects on Gut Microbiota and Immune Responses
Different dietary patterns significantly influence the composition and function of the gut microbiota, subsequently impacting immune responses. Vegan and vegetarian diets, often rich in fruits, vegetables, and legumes, are typically associated with a higher diversity of gut bacteria and increased levels of beneficial bacteria likeBifidobacteria*. This can lead to improved immune regulation and reduced inflammation. Conversely, the ketogenic diet, characterized by very low carbohydrate and high fat intake, may lead to a less diverse gut microbiome with a potential shift towards bacteria associated with inflammation.
Similarly, low-carbohydrate diets, while sometimes beneficial for weight management, can negatively affect gut microbiota diversity if not carefully planned to include sufficient fiber and other essential nutrients. The long-term effects of these various dietary patterns on immune function are still under investigation, but it is clear that a balanced approach, considering the overall nutrient profile, is crucial.
The Impact of Fiber Intake on Gut Health and Immune Modulation
Dietary fiber is a non-digestible carbohydrate that serves as a primary food source for beneficial gut bacteria. Fiber intake is strongly correlated with gut microbiota diversity and abundance of beneficial bacteria. Increased fiber consumption promotes the production of short-chain fatty acids (SCFAs), such as butyrate, propionate, and acetate, which have numerous beneficial effects on gut health and immune function.
SCFAs strengthen the gut barrier, reduce inflammation, and modulate immune cell activity, contributing to a healthier immune response and reduced risk of inflammatory diseases. A diet lacking sufficient fiber can lead to a less diverse and less functional gut microbiome, potentially increasing susceptibility to infections and inflammatory conditions.
Sample Meal Plan for Gut Health and Immunity
A balanced meal plan focused on gut health and immune function should incorporate a variety of foods rich in prebiotics, probiotics, and other essential nutrients. This sample meal plan provides a general guideline; individual needs may vary.
- Breakfast: Overnight oats with berries, chia seeds, and a dollop of plain yogurt (probiotics).
- Lunch: Lentil soup with whole-grain bread (fiber, prebiotics).
- Dinner: Baked salmon with roasted vegetables (broccoli, Brussels sprouts, sweet potatoes) and quinoa (fiber, prebiotics).
- Snacks: Apple slices with almond butter (fiber, healthy fats), a small handful of almonds (healthy fats), kefir (probiotics).
Lifestyle Factors and Immune Support
Maintaining a healthy gut and a robust immune system isn’t solely about diet. Lifestyle choices significantly impact both, creating a synergistic relationship where positive habits reinforce each other. Neglecting these aspects can undermine even the most carefully planned dietary interventions. Understanding and implementing these lifestyle strategies is crucial for holistic well-being.
Stress Management Techniques and Their Influence on Gut Health and Immune Function
Chronic stress profoundly affects the gut-brain axis, disrupting the delicate balance of the gut microbiome. Elevated cortisol levels, a hallmark of stress, can alter gut permeability (“leaky gut”), leading to inflammation and increased susceptibility to infections. Effective stress management techniques, such as mindfulness meditation, deep breathing exercises, and yoga, help regulate cortisol production, promoting a healthier gut environment and a more resilient immune system.
Studies have shown that individuals practicing regular mindfulness meditation exhibit a more diverse and balanced gut microbiome compared to those experiencing chronic stress. This improved microbiome composition is linked to reduced inflammation and improved immune responses.
Sleep Quality’s Impact on Gut Microbiome Composition and Immune Responses
Adequate sleep is paramount for both gut health and immune function. During sleep, the body repairs and regenerates, including the gut lining and immune cells. Sleep deprivation disrupts this process, leading to changes in gut microbiome composition, often characterized by a decrease in beneficial bacteria and an increase in potentially harmful ones. This shift can trigger inflammation and weaken immune responses, increasing vulnerability to illness.
For example, individuals consistently getting less than six hours of sleep per night often show a reduced abundance of beneficial bacteria like
- Bifidobacteria* and
- Lactobacilli*, impacting their immune system’s ability to effectively fight off infections.
Regular Physical Activity and its Role in Maintaining a Healthy Gut and Strong Immunity
Regular physical activity promotes a healthy gut microbiome by increasing gut motility, improving nutrient absorption, and reducing inflammation. Exercise also stimulates the production of immune cells and enhances their activity, bolstering the body’s defense mechanisms. Studies have shown that individuals engaging in moderate-intensity exercise experience improvements in gut diversity and a reduction in inflammatory markers. Furthermore, regular physical activity can improve sleep quality, further enhancing both gut health and immune function, creating a positive feedback loop.
Actionable Lifestyle Strategies to Optimize Gut Health and Boost the Immune System, Gut health and immune system
Implementing these lifestyle strategies can significantly improve gut health and enhance immune function. Consistency is key for realizing long-term benefits.
- Prioritize 7-9 hours of quality sleep each night.
- Engage in at least 150 minutes of moderate-intensity aerobic exercise per week.
- Practice stress-reducing techniques like meditation, yoga, or deep breathing exercises daily.
- Limit alcohol consumption and avoid smoking.
- Stay hydrated by drinking plenty of water throughout the day.
- Spend time in nature, connecting with the outdoors.
- Maintain a healthy weight through balanced nutrition and regular physical activity.
- Prioritize social connections and cultivate strong relationships.
Healthy Recipes and Cooking Tips
Nourishing your gut and bolstering your immune system relies heavily on the foods you consume. Choosing nutrient-rich ingredients and employing mindful cooking techniques can significantly impact your overall health. This section details three healthy recipes—one vegan, one vegetarian, and one keto-friendly—along with practical cooking tips to maximize nutrient retention and incorporate prebiotics and probiotics. A sample weekly meal plan integrating these strategies is also provided.
Vegan Gut-Boosting Bowl
This recipe is packed with prebiotic fiber and antioxidants, supporting both gut health and immunity.
Ingredients:
- 1 cup cooked quinoa
- 1 cup roasted sweet potatoes (cubed)
- 1/2 cup cooked lentils
- 1/2 cup chopped kale
- 1/4 cup chopped red onion
- 1/4 cup toasted pumpkin seeds
- 2 tablespoons tahini dressing (tahini, lemon juice, water, garlic)
Instructions:
Combine all ingredients in a bowl and toss gently with the tahini dressing. Enjoy warm or cold.
Vegetarian Lentil Soup with Turmeric
Lentils are an excellent source of prebiotic fiber, while turmeric possesses potent anti-inflammatory properties.
Ingredients:
- 1 cup brown or green lentils, rinsed
- 4 cups vegetable broth
- 1 medium onion, chopped
- 2 carrots, chopped
- 2 celery stalks, chopped
- 1 teaspoon turmeric
- 1/2 teaspoon cumin
- Salt and pepper to taste
Instructions:
Sauté onion, carrots, and celery in a large pot until softened. Add lentils, vegetable broth, turmeric, and cumin. Bring to a boil, then reduce heat and simmer for 30-40 minutes, or until lentils are tender. Season with salt and pepper.
Keto-Friendly Salmon with Asparagus and Avocado
This recipe is rich in healthy fats, omega-3 fatty acids, and vitamins, all beneficial for gut and immune function. Avocado provides healthy fats and fiber.
Ingredients:
- 2 salmon fillets (skin on or off)
- 1 bunch asparagus, trimmed
- 1 avocado, sliced
- 2 tablespoons olive oil
- Salt and pepper to taste
- Lemon wedges (optional)
Instructions:
Preheat oven to 400°F (200°C). Toss asparagus with 1 tablespoon olive oil, salt, and pepper. Roast for 10-12 minutes. Meanwhile, heat remaining olive oil in an oven-safe skillet. Season salmon with salt and pepper.
Cook salmon in the skillet for 3-4 minutes per side, then transfer to the oven and bake for another 5-7 minutes, or until cooked through. Serve salmon with roasted asparagus and avocado slices. Squeeze lemon juice over the salmon if desired.
Cooking Tips for Maximizing Nutrient Retention
Steaming, stir-frying, and baking are generally preferred cooking methods as they help retain more nutrients compared to boiling or frying. Minimizing cooking time also helps preserve vitamins and antioxidants. Adding herbs and spices not only enhances flavor but also provides additional health benefits.
Incorporating Prebiotics and Probiotics into Everyday Meals
Prebiotics (fiber) are found in foods like onions, garlic, bananas, and asparagus. Probiotics (live beneficial bacteria) are present in fermented foods such as yogurt, kefir, sauerkraut, and kimchi. Incorporate these foods into your daily diet to support gut health. Consider adding a probiotic supplement if needed, but always consult a healthcare professional.
Weekly Meal Plan
This is a sample plan and can be adjusted based on your preferences and dietary needs.
- Monday: Vegan Gut-Boosting Bowl
- Tuesday: Vegetarian Lentil Soup with Turmeric, whole-wheat bread
- Wednesday: Leftover Lentil Soup, side salad
- Thursday: Keto-Friendly Salmon with Asparagus and Avocado, side of green beans
- Friday: Chicken stir-fry with plenty of vegetables (broccoli, peppers, onions), brown rice
- Saturday: Homemade pizza with whole-wheat crust, lots of vegetables, and a sprinkle of probiotic-rich sauerkraut
- Sunday: Breakfast: Yogurt with berries and granola; Lunch: Leftover pizza; Dinner: Baked chicken breast with roasted sweet potatoes and a side of kimchi.
Vegan and Vegetarian Diets for Gut Health
Plant-based diets, encompassing vegan and vegetarian approaches, are increasingly recognized for their potential to positively influence gut health and, consequently, the immune system. This stems from the high fiber content and diverse array of phytochemicals found in plant-based foods. However, careful planning is essential to ensure adequate nutrient intake and avoid potential deficiencies.
Potential Benefits and Challenges of Vegan and Vegetarian Diets for Gut Health and Immunity
Vegan and vegetarian diets, characterized by high fiber intake from fruits, vegetables, legumes, and whole grains, promote a diverse gut microbiota. This diversity is crucial for robust gut health and a strong immune response. Fiber acts as prebiotic fuel, fostering the growth of beneficial bacteria. Furthermore, plant-based diets often contain a wealth of polyphenols and other bioactive compounds with anti-inflammatory properties, potentially mitigating gut inflammation and supporting immune function.
However, challenges exist. Vegan diets, in particular, require careful attention to ensure sufficient intake of vitamin B12, vitamin D, iron, zinc, calcium, and omega-3 fatty acids, nutrients often found in higher concentrations in animal products. Careful meal planning and supplementation may be necessary to address these potential deficiencies. Vegetarian diets, while generally easier to manage nutritionally, still require attention to iron and calcium intake.
Nutritional Considerations for Vegan and Vegetarian Diets
Meeting nutritional needs on a vegan or vegetarian diet requires mindful food choices and potentially supplementation. Iron deficiency is a common concern, as plant-based iron (non-heme iron) is less readily absorbed than heme iron from animal sources. Pairing iron-rich foods like lentils or spinach with vitamin C-rich foods like citrus fruits or bell peppers enhances absorption. Similarly, calcium intake needs attention, as dairy is excluded from vegan diets.
Good sources of calcium include leafy greens, fortified plant milks, and tofu. Vitamin B12 is crucial and is not naturally found in plant-based foods, requiring supplementation or consumption of fortified foods. Omega-3 fatty acids, typically found in fish oil, can be obtained from plant-based sources like flaxseeds and chia seeds, though their conversion to the active forms in the body is less efficient.
Zinc, another essential mineral, is also present in lower concentrations in plant-based foods compared to animal products, so careful attention to intake is necessary.
Examples of Vegan and Vegetarian Recipes Rich in Prebiotics and Probiotics
Prebiotics and probiotics are essential for a healthy gut. Here are some examples of recipes incorporating these elements:
Lentil Soup with Kimchi
Ingredients: Brown or green lentils, vegetable broth, carrots, celery, onions, garlic, kimchi (fermented cabbage), ginger, soy sauce (or tamari for gluten-free), and spices. Instructions: Sauté vegetables, add lentils and broth, simmer until lentils are tender. Stir in kimchi and spices before serving. Kimchi provides probiotics, and lentils are a good source of prebiotic fiber.
Vegan Miso Soup with Shiitake Mushrooms
Ingredients: Miso paste (fermented soybean paste), vegetable broth, shiitake mushrooms, tofu, seaweed (wakame or kombu), scallions. Instructions: Simmer broth with mushrooms, add tofu and seaweed. Stir in miso paste just before serving to retain its beneficial bacteria. Miso paste is rich in probiotics, and shiitake mushrooms provide prebiotic fiber.
Resources for Planning Balanced Vegan and Vegetarian Meals
Planning balanced vegan and vegetarian meals can be easier with the help of various resources:
- Registered Dietitians specializing in plant-based nutrition: They can provide personalized guidance.
- Websites and apps focusing on vegan and vegetarian recipes: Many offer meal planning tools and nutritional information.
- Cookbooks dedicated to plant-based cuisine: These offer a wealth of recipe ideas.
- Online communities and forums for vegans and vegetarians: These provide support and recipe sharing.
Keto and Low-Carb Diets and Gut Microbiota: Gut Health And Immune System
Ketogenic and low-carbohydrate diets, characterized by drastically reduced carbohydrate intake and increased fat consumption, have gained popularity for weight loss and other health benefits. However, their impact on the gut microbiome, a complex community of microorganisms residing in the digestive tract, is a subject of ongoing research and debate. Understanding this impact is crucial because the gut microbiome plays a vital role in overall health, including immune function.The shift in macronutrient intake inherent in keto and low-carb diets significantly alters the gut environment.
Reduced carbohydrate availability limits the growth of certain bacterial species that thrive on carbohydrates, potentially leading to a decrease in microbial diversity. Conversely, increased fat intake might favor the growth of bacteria that can metabolize fats. This alteration in microbial composition can have both positive and negative consequences for gut health and, subsequently, the immune system.
Impact on Gut Microbiome Composition
Studies have shown mixed results regarding the impact of ketogenic diets on gut microbiota composition. Some research indicates a reduction in beneficial bacteria like Bifidobacteria and Lactobacilli, while others observe an increase in certain types of bacteria associated with inflammation. The variability in findings may be due to differences in study design, participant characteristics, and the specific dietary protocols employed.
Long-term studies are needed to fully understand the long-term consequences of these dietary patterns on the gut microbiome. For example, a study comparing the gut microbiota of individuals on a ketogenic diet for six months versus a control group found a significant decrease in butyrate-producing bacteria in the keto group. Butyrate is a short-chain fatty acid with anti-inflammatory properties, highlighting a potential negative consequence of long-term adherence to a ketogenic diet.
Immune Function Modulation
The gut microbiome profoundly influences the immune system. Changes in its composition, triggered by ketogenic diets, can affect immune responses. While some studies suggest potential benefits, such as reduced inflammation in specific contexts, others raise concerns about increased susceptibility to certain infections due to altered immune regulation. The long-term effects on immune function remain largely unclear and require further investigation.
For instance, a decrease in butyrate-producing bacteria could potentially contribute to chronic low-grade inflammation, which is implicated in various diseases. Conversely, a potential benefit might be seen in individuals with specific autoimmune disorders where reducing inflammation is crucial.
Long-Term Effects Compared to Other Diets
Compared to balanced diets rich in fruits, vegetables, and whole grains, keto and low-carb diets may lead to less diverse gut microbiomes in the long term. Diets emphasizing plant-based foods generally promote a more diverse and robust gut microbiome, supporting a healthier immune system. The long-term consequences of reduced microbial diversity associated with ketogenic diets are still being investigated, but a less diverse microbiome is often linked to an increased risk of various health problems.
More research is needed to definitively compare the long-term effects of these diets on gut health.
Potential Risks and Benefits
Potential risks associated with keto and low-carb diets regarding gut health include reduced microbial diversity, potential imbalances in gut microbiota composition, and increased susceptibility to infections. However, potential benefits may include reduced inflammation in certain individuals and improved metabolic parameters that could indirectly benefit gut health. The overall risk-benefit profile varies greatly depending on individual factors, such as pre-existing health conditions and the specific dietary protocol followed.
Strategies to Mitigate Negative Impacts
To mitigate potential negative impacts on gut health while following keto or low-carb diets, individuals can focus on strategies to support a healthy microbiome. This includes consuming foods rich in prebiotics (fibers that feed beneficial bacteria) such as resistant starches (found in some vegetables and cooked and cooled potatoes) and inulin (found in chicory root), and incorporating fermented foods like yogurt and kefir (containing probiotics) in moderation.
Adequate hydration and managing stress are also crucial for optimal gut health. Furthermore, regular monitoring of gut health markers and seeking guidance from a registered dietitian or healthcare professional is recommended, especially for individuals with pre-existing health conditions.
Intermittent Fasting and Gut Health

Intermittent fasting (IF), characterized by cyclical periods of eating and voluntary fasting, is gaining popularity as a dietary strategy for weight management and overall health. Emerging research suggests that IF may also significantly impact gut microbiota composition and function, with potential implications for immune responses. This section explores the mechanisms by which IF influences gut health and immunity, examines potential benefits and drawbacks, and provides guidelines for safe and effective implementation.Intermittent fasting’s effects on the gut microbiome are multifaceted and not fully understood.
However, studies suggest that periods of fasting can trigger changes in the gut environment, leading to shifts in the types and abundance of gut bacteria. These changes are thought to be mediated by several mechanisms, including alterations in nutrient availability, changes in gut hormone production, and modifications to the gut’s immune system. For instance, fasting can lead to a reduction in inflammation, which may benefit individuals with inflammatory bowel diseases.
Conversely, improperly implemented IF could potentially disrupt the delicate balance of the gut microbiome, leading to negative consequences.
Mechanisms of Intermittent Fasting’s Impact on Gut Microbiota and Immune Responses
The impact of intermittent fasting on the gut microbiome is complex and involves several intertwined mechanisms. Reduced nutrient availability during fasting periods can alter the composition of the gut microbiota, favoring bacteria that are more resilient to nutrient scarcity. This can lead to a shift towards a more diverse microbiome, which is generally associated with better health. Furthermore, fasting induces changes in the production of gut hormones, such as ghrelin and peptide YY, which play a role in regulating appetite and metabolism, and may indirectly affect the gut microbiome and immune function.
Finally, fasting can influence the activity of immune cells within the gut, potentially reducing inflammation and promoting a healthier gut environment. For example, some studies suggest that IF may reduce the levels of pro-inflammatory cytokines, thus mitigating inflammatory responses in the gut.
Potential Benefits and Drawbacks of Intermittent Fasting for Gut Health and Immunity
While research is ongoing, several potential benefits of intermittent fasting for gut health and immunity have been identified. These include improved gut barrier function, reduced inflammation, and increased microbial diversity. A stronger gut barrier helps prevent the leakage of harmful substances into the bloodstream, thus reducing the risk of systemic inflammation. The reduction in inflammation can be particularly beneficial for individuals with inflammatory bowel diseases (IBD) like Crohn’s disease and ulcerative colitis.
Increased microbial diversity contributes to a more resilient and balanced gut ecosystem, better equipped to withstand environmental challenges and pathogens. However, intermittent fasting is not without potential drawbacks. Improperly implemented IF, such as overly restrictive fasting periods or inadequate nutrient intake during eating windows, can negatively impact gut health by disrupting the microbiome balance and potentially leading to nutrient deficiencies.
Individuals with certain medical conditions, such as eating disorders or those taking specific medications, should consult their healthcare provider before starting intermittent fasting.
Guidelines for Safe and Effective Intermittent Fasting Practices
Safe and effective intermittent fasting requires careful planning and consideration of individual needs. It’s crucial to prioritize gradual implementation to allow the body to adapt. Beginners should start with shorter fasting periods and gradually increase the duration as tolerated. Maintaining adequate hydration throughout the fasting period is vital, as dehydration can exacerbate negative effects. Focusing on nutrient-dense foods during eating windows is essential to prevent nutrient deficiencies.
A balanced diet rich in fruits, vegetables, whole grains, and lean proteins is recommended. Listening to your body’s signals is crucial; if you experience any adverse effects such as dizziness, fatigue, or severe hunger, you should adjust your fasting schedule or discontinue IF altogether. Regular monitoring of weight, blood glucose levels, and overall well-being is recommended, particularly for individuals with pre-existing health conditions.
Incorporating Intermittent Fasting into a Healthy Lifestyle
Successfully integrating intermittent fasting into a healthy lifestyle requires a structured approach. Consider these guidelines:
- Choose a Suitable Fasting Protocol: Explore different methods like the 16/8 method (16 hours fasting, 8 hours eating window), the 5:2 diet (five normal eating days, two restricted calorie days), or alternate-day fasting, and select one that aligns with your lifestyle and preferences. Start slowly and gradually increase the duration of fasting.
- Prioritize Nutrient Density: During your eating window, focus on consuming nutrient-rich foods. Prioritize whole, unprocessed foods, including fruits, vegetables, lean proteins, and healthy fats. Avoid processed foods, sugary drinks, and excessive refined carbohydrates.
- Stay Hydrated: Drink plenty of water, herbal tea, or black coffee throughout the day, especially during fasting periods. Avoid sugary drinks.
- Listen to Your Body: Pay attention to your hunger and energy levels. If you experience any negative side effects, such as dizziness, fatigue, or irritability, adjust your fasting schedule or consult a healthcare professional.
- Combine with Regular Exercise: Incorporate regular physical activity into your routine. Exercise can help improve overall health and well-being and may enhance the benefits of intermittent fasting.
- Monitor Your Progress: Track your weight, energy levels, and any other relevant health markers to monitor your progress and make adjustments as needed. Regular check-ups with your healthcare provider are recommended.
In conclusion, nurturing a healthy gut microbiome is paramount for a robust immune system. The bidirectional communication between these two systems highlights the importance of a holistic approach to wellness. By adopting a balanced diet rich in prebiotics and probiotics, incorporating stress-reducing techniques, prioritizing sleep, and engaging in regular physical activity, we can significantly enhance both gut health and immune function, paving the way for improved overall health and well-being.
The journey to a stronger immune system begins with a healthy gut.
FAQs
What are the signs of an unhealthy gut?
Common signs include bloating, gas, constipation, diarrhea, abdominal pain, and fatigue. Skin issues like acne or eczema can also be indicative of gut imbalances.
Can antibiotics negatively impact gut health?
Yes, antibiotics can disrupt the balance of the gut microbiome, potentially leading to gut dysbiosis and increased susceptibility to infections.
How long does it take to see improvements in gut health after making dietary changes?
The timeframe varies depending on individual factors and the extent of the changes. Some people notice improvements within weeks, while others may see significant changes after several months.
Are all probiotics created equal?
No, different probiotic strains have different effects on the body. The effectiveness of a probiotic depends on the specific strain and individual factors.






